Do you feel a sharp pain in your heel as soon as you put your foot on the ground in the morning or after a prolonged walk? This discomfort, sometimes compared to a stinging sensation or a bruise under the heel, can greatly disrupt your daily activities. These symptoms are often indicative of several common foot conditions. Find out how to precisely identify your condition and access the right solutions at Médecine podiatrique du Plateau, in the heart of the AGORA complex in Gatineau.
Common causes of heel pain
Heel pain can occur for a variety of reasons, often related to lifestyle habits or recent changes in your routine. Understanding these triggering factors allows us to quickly direct the patient to the right diagnosis.
Biomechanical and postural factors
- Sudden weight gain: Weight gain, whether it’s related to pregnancy, a period of stress, or rapid bulking, puts extra pressure on the feet. This can lead to overloading of the plantar fascia, which causes inflammation and pain.
- Wearing unsuitable shoes: Flat shoes, unsupportive sandals, or ill-fitting shoes can compromise the natural alignment of the foot. Without proper arch support, the pressure on the heel increases, leading to chronic injuries.
- Increased physical activity: Transitioning from a sedentary lifestyle to a high-intensity workout, running on hard surfaces, or playing demanding sports like tennis or basketball can quickly overwork the plantar fascia and cause strain injuries.
- Prolonged standing at work: Occupations that require standing for several hours, such as retail or catering, strain the soft tissues of the foot, increasing the risk of chronic inflammation.
- Sports injuries: Repeated impacts or false movements, common in sports activities, can cause microcracks or lesions that affect the heel.
These situations put excessive pressure on the plantar fascia or promote bone calcifications. Early attention and habit adjustment can prevent these pains from getting worse.
Pain under the heel: identifying the exact area
The precise location of your pain is a key element in the diagnosis. Pain under the heel has distinct characteristics that point to specific conditions.
Typical area of presentation
- In the center of the footridge of the heel
- Under the calcaneus bone (heel bone)
- Sometimes extended to the arch of the foot
Characteristics of pain under the heel
Patients typically describe:
- Feeling of “stepping on a nail” or “pebble in the shoe”
- Maximum pain on the first steps in the morning
- Gradual improvement after a few minutes of walking
- Recurrence after prolonged sitting
- Intensification at the end of the day after standing
Main causes of pain under the heel
Pain under the heel typically results from:
Plantar fasciitis (plantar fasciopathy, plantar fasciopathy)
Inflammation of the plantar fascia, the thick tissue that supports the arch of the foot. It is the most common cause of pain under the heel, affecting about 10% of the adult population during their lifetime.
Heel Spur
Bone calcification in the heel, often associated with chronic plantar fasciitis. Visible on X-rays, it is not always symptomatic in itself.
Foot pad atrophy
Progressive thinning of fatty tissue under the heel, more common after the age of 50. This natural aging phenomenon reduces shock absorption.
Poor foot biomechanics
Excessive pronation, excessive supination (high arches), or flat foot can create an uneven distribution of pressure, overloading certain areas of the heel.
When to worry?
Consult a podiatrist promptly if:
- Pain persists for more than 2 weeks despite rest
- Discomfort gradually increases
- You limp to avoid pressing on the heel
- Redness or swelling appears
- Pain wakes you up at night
Dr. Émile Carrier, podiatrist, recommends a complete assessment including X-rays and ultrasound to precisely identify the origin of your pain under the heel.
Back heel pain: a different problem
Unlike pain under the heel, pain in the back of the heel often indicates distinct conditions that require a different therapeutic approach.
Typical area of presentation
- Posterior part of the heel
- Above the Achilles tendon insertion
- On the sides of the hindfoot
Common conditions at the back of the heel
1. Achilles tendonitis
Description: Inflammation of the Achilles tendon, the largest tendon in the human body, connecting the calf muscles to the heel bone.
Characteristic symptoms:
- Pain along the tendon behind the heel
- Significant morning stiffness, improving with warm-up
- Discomfort that increases with physical activity
- Sometimes visible swelling of the tendon
- Crackling sensation on palpation
Risk factors: Sudden increase in activity, lack of stretching, unsuitable shoes, change of training surface.
2. Retrocalcaneal bursitis
Description: Inflammation of the bursa located between the Achilles tendon and the calcaneal bone. This small pouch filled with liquid normally acts as a protective pad.
Characteristic symptoms:
- Deep pain behind the heel
- Aggravated by the pressure of closed shoes
- Visible and palpable localized swelling
- Redness of the skin in cases of acute inflammation
- Pain when flexion the foot
3. Haglund deformation
Description: Bony growth at the back of the calcaneus, creating a visible prominence. Often called a “pump bump” because it is frequently caused by wearing rigid shoes including skates and downhill ski boots.
Characteristic symptoms:
- Visible and palpable hump at the back of the heel
- Painful friction with closed shoes
- Callus formation on the prominence
- Recurrent inflammation of the adjacent bursa
Warning signs requiring prompt consultation
- Inability to stand on tiptoe
- Severe nocturnal pain
- Change in skin colour (significant redness)
- Marked local warmth
- Significant claudication
Key Differences: Pain Under vs Back of the Heel
| Criterion | Pain UNDER the heel | BACK heel pain |
|---|---|---|
| Most painful | First steps in the morning | During and after the activity |
| Structure involved | Plantar | Achilles tendon/bursa |
| Main | X-ray + Foot | Tendon ultrasound (MRI if needed) |
| Priority | Foot orthotics + stretching | Stretching + shoe modifications |
| Improvement with walking | Yes, often | Variable, sometimes worsening |
A comprehensive biomechanical evaluation at our clinic makes it possible to precisely differentiate these conditions and adapt the treatment accordingly.
Heel spurs or plantar fasciitis: what are the differences?
The heel spur
What is it?
The heel spur is a bony calcification that develops in the heel, usually under the calcaneal bone. It forms as a result of repeated microtrauma or excessive pressure on this sensitive area, often caused by prolonged posture, overweight or intense physical exertion.
This bone growth can remain painless in some cases, but becomes problematic when combined with inflammation of the surrounding tissues, such as the plantar fascia. About 50% of people with a heel spur visible on an x-ray do not feel any pain.
Symptoms
The main sign of heel spurs is calcification visible on x-ray. When there is no associated pain, treatment is usually not necessary. In the presence of localized and acute pain in the heel, particularly felt after a prolonged period of rest, such as when waking up or after sitting for a long time, it is called associated plantar fasciitis.
This pain is often described as a stinging or burning sensation, which gradually subsides as the day progresses with activity.
Diagnosis
An accurate diagnosis requires an X-ray, which allows the bone growth to be directly visualized. This examination is rapid, non-invasive and performed on site at Médecine podiatrique du Plateau, allowing for a clear and immediate evaluation.
In-clinic treatment
Depending on the severity and associated symptoms, treatments such as custom-made foot orthotics, cortisone injections or shoe modifications are offered to reduce discomfort. The results vary according to the condition of each person and compliance with the treatment plan.
Plantar fasciitis
What is it?
Plantar fasciitis is an inflammation of the plantar fascia, a thick, fibrous tissue that extends from the heel to the base of the toes. This tissue plays a key role in supporting the arch of the foot and absorbing shock when walking or running.
When subjected to excessive tension or repeated microtrauma, it becomes inflamed, causing sometimes debilitating pain under the foot. Plantar fasciitis accounts for more than 15% of all podiatric consultations.
Symptoms
People with plantar fasciitis usually experience sharp, throbbing pain underfoot, often concentrated near the heel. This pain is particularly intense when you get up, after a night’s rest and tends to subside with activity before reappearing after a prolonged day or physical exertion.
In some cases, it can be diffuse, extending to the entire arch of the foot. Patients often describe the “first steps in the morning” as the most difficult.
Diagnosis
The diagnosis is based on a musculoskeletal ultrasound, which visualizes inflammation and assesses the thickness of the plantar fascia. A normal fascia is about 3-4 mm thick; in case of fasciitis, it can exceed 5-6 mm.
This rapid and non-invasive examination is carried out directly on site at Médecine podiatrique du Plateau, allowing a precise and personalized diagnosis during your first visit.
In-clinic treatment
Solutions include specific stretching exercises, tapings to support the fascia, custom-made foot orthotics, targeted injections, physical therapies such as Class IV therapeutic laser, and shoe adjustments to limit tension. A gradual treatment plan usually allows for an improvement in discomfort over 6 to 12 weeks. Results vary depending on initial severity and adherence to the protocol.
Heel bursitis: the little-known inflammation
Bursitis is an inflammation of the bursa, small fluid-filled sacs that act as cushions between bones, tendons and muscles. Although often confused with plantar fasciitis, it requires a distinct therapeutic approach.
Types of Heel Bursitis
1. Retrocalcaneal bursitis (back of the heel)
Location: Located between the Achilles tendon and the calcaneus bone
Main causes:
- Repeated pressure from rigid shoes (high heels, new running shoes)
- Excessive friction during sports activities
- Underlying Haglund deformation
- Sudden increase in training volume
Population at risk: Common in long-distance runners, active walkers, and people who regularly wear high heels.
2. Subcalcaneal bursitis (under the heel)
Location: Inflammation under the heel bone
Main causes:
- Natural fat tissue atrophy (more common after age 40)
- Direct trauma (fall on heels, jump from a height)
- Prolonged standing on hard surfaces
- Wearing shoes with soles that are too thin
Key distinction: Often confused with plantar fasciitis, but the pain is more diffuse and less concentrated on the inner edge of the heel.
Distinctive symptoms of bursitis
- Localized and deep pain (vs. “band” pain of fasciitis)
- Visible swelling at the site of inflammation
- “deflated cushion” feeling under the heel
- Pain on direct pressure (thumb test)
- Constant discomfort, not just at the first steps
- Local heat in case of acute inflammation
Triggers and aggravating factors
- Poorly fitting shoes (too tight at the back, stiff heel counter)
- Sudden increase in physical activity without gradual adaptation
- Direct trauma (blow, fall, accident)
- Underlying inflammatory arthritis (rheumatoid arthritis, spondyloarthritis)
- Obesity or rapid weight gain
Diagnosis at our clinic
Targeted musculoskeletal ultrasound is the reference diagnostic tool. It allows you to:
- Visualize the inflammation of the bursa
- Measure tissue thickening (normal < bursa 2mm)
- Distinguish bursitis and plantar fasciitis accurately
- Detect any calcifications or bone growths
- Assess the condition of the adjacent Achilles tendon
Our podiatrists have advanced training in musculoskeletal ultrasound, allowing for an accurate diagnosis during your visit.
Treatment Options
Prognosis and recovery times
Most patients report a gradual improvement in discomfort over 4 to 8 weeks with an appropriate treatment plan. The results vary according to:
- The initial severity of the inflammation
- The presence of underlying conditions
- Compliance with the treatment protocol
- Lifestyle adjustments (shoes, activities)
Chronic bursitis (> 6 months) may require more prolonged treatment and a multidisciplinary approach.
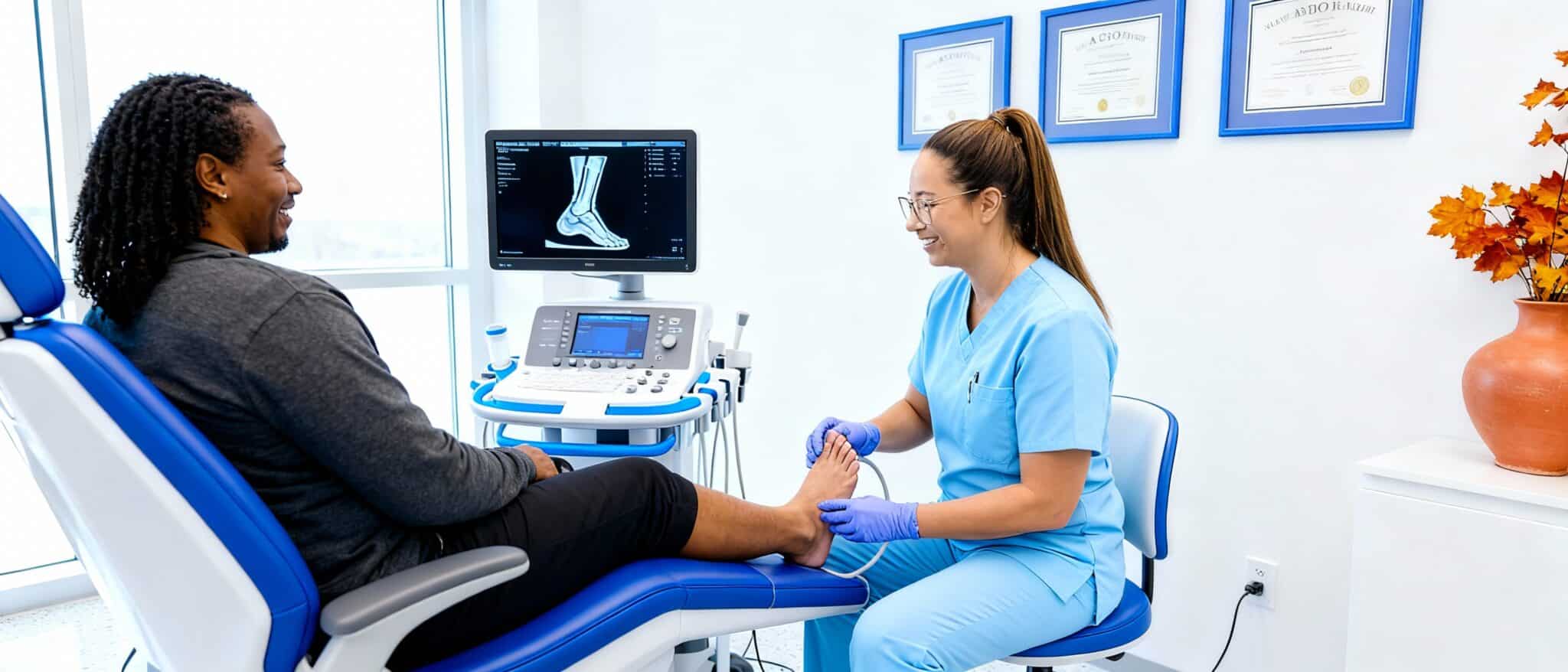
Why consult a podiatrist for your heel pain?
Many people try to endure their heel pain or treat themselves with home remedies for months. An early podiatric consultation significantly changes the prognosis and accelerates the return to your activities.
Accurate medical diagnosis
Unlike generic online advice, our podiatrists:
- Assess your complete biomechanics (gait analysis, posture, balance)
- Identify the exact cause via medical imaging (X-ray, ultrasound)
- Differentiate between multiple possible conditions (fasciitis, bursitis, stress fracture, neuroma)
- Detect contributing factors (muscle imbalance, poor posture, systemic pathologies)
- Establish an evidence-based treatment plan
The right treatment, fast
Avoiding aggravation
Untreated plantar fasciitis can:
- Becoming chronic (recovery time multiplied by 3 to 4)
- Cause compensatory pain (knee, hip, lumbar region)
- Developing partial fascia tears
- Lead to progressive atrophy of the foot pad
- Creating difficult-to-treat calcifications
Access to advanced technologies
At Médecine podiatrique du Plateau, in the heart of the AGORA complex in Gatineau:
- Digital X-ray on site: Immediate results, reduced exposure
- Targeted musculoskeletal ultrasound: Real-time visualization of soft tissues
- Class IV therapeutic laser: Health Canada licensed, clinically validated protocols
- Shockwave therapy : regenerative treatment that is particularly useful for long-standing pain.
- 3D Digital Impressions: Optimal precision for custom orthotics
- Computerized biomechanical analysis: Objective evaluation of your approach
When to consult: the practical guide
🔴 Consult within 48-72 hours if:
- Sudden and severe pain after identifiable trauma
- Inability to put weight on the heel
- Severe swelling with marked redness and warmth
- Night pain that wakes you up regularly
- Visible deformity of the foot or heel
We accept minor emergencies and can usually see you the same day or the next day.
🟡 Consult within 1-2 weeks if:
- Persistent morning pain for more than 7 days
- Discomfort that makes you limp or change your gait
- Progressive limitation in your daily activities
- Ineffective self-treatment after 10-14 days
- Pain that intensifies despite rest
🟢 Make an appointment for evaluation if:
- Intermittent pain for several months
- Recurrence of pain despite previous treatments
- Concern about a podiatric condition
- Desire for prevention (preventive biomechanical assessment)
- Planning of intense sports activities
What happens on your first visit
Your initial consultation at Médecine podiatrique du Plateau takes place in four structured steps:
1. Complete history (approximately 10 minutes)
- In-depth discussion of your symptoms and medical history
- Identification of triggers and aggravating factors
- Assessing your activity level and goals
- Review of your usual shoes
2. Biomechanical examination (approximately 15 minutes)
- Analysis of your static and dynamic posture
- Flexibility and muscle strength tests
- Joint Range of Motion Assessment
- Precise palpation of painful areas
- Observation of your gait (gait analysis)
3. Imaging if necessary
- X-ray for heel spurs, fracture or osteoarthritis
- Ultrasound for fasciitis, bursitis, or tendonitis
- Immediate Outcomes and Interpretation
- Note that an ultrasound examination requires an extended period of time and will often be performed during a separate visit.
4. Personalized treatment plan (10 minutes)
- Clear explanation of diagnosis in accessible terms
- Treatment options tailored to your situation
- Realistic goals and recovery timelines
- Provision of written documentation
- Answers to all your questions
What a podiatrist can do
As health professionals, our podiatrists have distinct skills:
- Medical prescriptions: Foot orthotics, topical medications, medical imaging, laboratory tests
- Specialized interventions: Therapeutic injections, physical therapies such as manual therapy, therapeutic laser and radial shock waves, minor foot surgeries
- Therapeutic adjustments: Modification of orthotics, adaptation of protocols according to evolution
- Differential diagnosis: Elimination of systemic, neurological or vascular causes
- Interprofessional collaboration: Communicating with your family doctor, physiotherapist or specialist
Invest in your feet, invest in your mobility
Your feet support the equivalent of 120% of your body weight with each step. On an average day of 8,000 steps, this represents more than 1.5 million kg of cumulative pressure. Ignoring heel pain is compromising your future independence and quality of life.
Important fact: Heel pain treated early (< 6 weeks) usually resolves within 6 to 12 weeks. If left untreated, they can persist for months or even years and require more invasive interventions. The results vary according to the condition of each person.
3 treatments to try at home while waiting for your consultation
While waiting to see a podiatrist to evaluate your heel pain, a few simple things you can do at home can provide real relief. These methods help reduce inflammation, relax the tissues underfoot, and temporarily ease discomfort.
1. Apply ice
Ice is a great way to calm inflammation and reduce pain.
Method: Take a bottle of ice water, put it under your foot and roll it gently for 10 minutes, three times a day. This movement not only soothes the pain, but also massages the plantar fascia, reducing the accumulated tension.
Important: Never apply ice directly to the skin. Use a thin towel if necessary.
2. Wear suitable shoes
Absolutely avoid walking barefoot or in flat shoes that offer no support.
Characteristics of a good shoe:
- Built-in arch support
- Slightly raised heel (1.5 to 2.5 cm)
- Stiff sole that doesn’t bend easily in the middle
- Firm rear heel counter for stability
- Sufficient toe room
Avoid: Flat sandals, flip-flops, “minimalist” type shoes, slippers without support.
Crucial Tip: You should wear these shoes from the moment you get out of bed, even for a few steps.
3. Use a tennis ball
To relax the plantar fascia and reduce pain, gently roll a tennis ball under your foot for 3-5 minutes, 2-3 times a day.
Technique: Sitting comfortably, apply moderate pressure by rolling the ball from the heel to the toes. Focus on sensitive areas without overly exercising.
Benefits: This exercise helps improve blood circulation, reduce muscle tension, and stimulate sore tissue.
Important note: These simple treatments, combined with adapted habits, can improve your comfort temporarily, but are not a substitute for a professional evaluation. If the pain persists for more than 2 weeks or worsens, a consultation is necessary to identify the exact cause and receive appropriate treatment.
Why choose Médecine podiatrique du Plateau?
When you suffer from heel pain, an accurate diagnosis and the right treatments make all the difference. At Médecine podiatrique du Plateau, we provide you with an experienced team and modern equipment to offer you personalized and effective care.
A team of experienced podiatrists
Our clinic brings together three podiatrists with complementary skills:
- Dr. Émile Carrier, podiatrist: licensed in Quebec and Ontario, training in musculoskeletal ultrasound, involved in university research on the implementation of local foot health services in Quebec, co-owner
- Dr. Sandra Gendron, podiatrist: Training in New York, integrative approach, co-owner
- Dr. Stephen Davis, podiatrist: 15 years of experience, practices in Quebec and Ontario, experience in manual therapy and in a podiatric clinic for foot surgery
Fast and accurate diagnosis
With our advanced tools such as X-ray and on-site ultrasound, we quickly identify the origin of your pain, whether it’s plantar fasciitis, heel spurs, bursitis, or another problem. This precise diagnosis allows you to set up a treatment plan that is perfectly adapted to your situation.
Tailor-made treatments to reduce your pain
Custom Foot Orthotics
Designed specifically for your feet via 3D digital imprints, they provide optimal support, reduce pressure on the heel and correct biomechanical imbalances. Manufacturing time: about 3 weeks.
Class IV Therapeutic Laser
This treatment helps to progress the injury through the healing stages more quickly by stimulating the supply of oxygen and increasing the speed of chemical reactions in the cells. Health Canada Licensed.
Radial shockwave
This treatment consists of applying high-intensity acoustic waves to the painful area of the foot. These waves stimulate blood circulation, promote tissue regeneration, and trigger a natural healing response.
Therapeutic exercises
Our podiatrists teach you simple and effective movements to strengthen the foot muscles, stretch the plantar fascia and reduce inflammation. Personalized program according to your requirement.
Bandages and tapings
These techniques limit tension on the plantar fascia and promote healing while immediately reducing discomfort. Immediate effect often felt upon application.
Cortisone injections
In case of severe inflammation that does not respond to conservative treatments, our podiatrists can administer targeted injections to quickly reduce pain and inflammation. Procedure generally well tolerated.
Hyaluronic acid injections
One of our podiatrists can inject a biocompatible hyaluronic acid adapted for soft tissues to not only relieve pain, but above all restore the function of injured tendons and ligaments. Although more expensive than the cortisone injection due to the cost of the product, this procedure has the advantage of being regenerative compared to cortisone, which attacks the pain more.
Advice on suitable shoes
We help you choose shoes that offer adequate support and minimize the risk of recurrence, taking into account your lifestyle and daily activities. Analysis of your current shoes included.
Human and professional support
At Médecine podiatrique du Plateau, we understand how much heel pain can disrupt your daily life. That’s why our team is committed to offering you personalized follow-up and practical advice to help you regain your comfort and mobility.
Our Location: In the Heart of Gatineau
Located at 20 Allée de Hambourg, Entrance A, 2nd floor, in the AGORA urban village in Gatineau, we are easily accessible for residents of Gatineau, Hull, Aylmer and Ottawa. Free parking available (3 hours, outdoor parking P1).
Book an appointment today
Don’t let heel pain limit your activities. Our podiatrists are ready to welcome you for a complete evaluation and a personalized treatment plan.
Phone: 819-800-1212
Website: podiatreplateau.com


