Ankle sprain: quick diagnosis and complete treatment in Gatineau
You walk on an uneven sidewalk. Your ankle twists sharply inwards. The shooting pain stops you immediately. You try to limp on your way. Swelling appears quickly.
You ask yourself, “Is this a big deal? Should I consult? Can I continue walking? »
Ankle sprains are one of the most common musculoskeletal injuries. Yet, many people minimize this injury and neglect proper treatment. This neglect often turns an acute sprain into chronic instability that persists for years.
At Médecine podiatrique du Plateau, Dr. Sandra Gendron, Dr. Stephen Davis and Dr. Émile Carrier, podiatrists evaluate and treat ankle sprains with advanced diagnostic technologies. Our clinic is located at the AGORA complex in Gatineau (Plateau sector). X-ray and musculoskeletal ultrasound on site. We offer you personalized care and treatment plan. The goal? A complete rehabilitation.
This guide helps you understand ankle sprain, recognize its severity, and discover treatment options that speed up your recovery.
What is an ankle sprain?
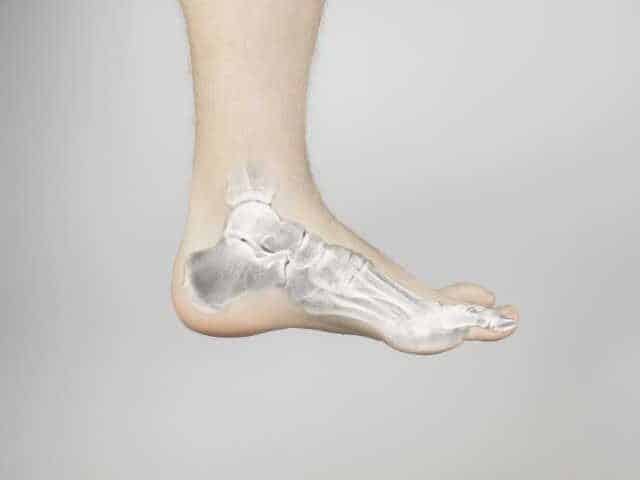
A sprain occurs when the ligaments stabilizing your ankle are overstretched or torn. Ligaments are bands of strong connective tissue that hold bones together. Unlike muscles that actively contract, ligaments provide passive but essential support.
Lateral (external) ankle sprain accounts for 85% of cases. Your foot turns inward abruptly (inversion), stretching or tearing the ligaments on the outside of the ankle. The anterior talofibular ligament suffers the most frequent damage, followed by the calcaneofibular ligament.
Sprains are classified according to their severity.
Grade 1 (mild): ligament stretch without significant tearing, moderate pain, minimal swelling, ability to walk retained.
Grade 2 (moderate): partial tear of ligaments, marked pain, significant swelling, difficulty walking, mild instability.
Grade 3 (severe): complete tear of one or more ligaments, severe pain, massive swelling, inability to support weight, significant instability.
Sprains and strains: synonyms for the same injury
These terms refer to the same injury and are often used interchangeably. Sprains (or strains) affect the ligaments that connect the bones together. When your ankle twists, the ligaments overstretch or tear.
This terminological confusion sometimes stems from popular usage where some people use “strain” to describe a mild sprain and “sprain” for a more severe injury. In reality, it is the same type of ligament injury, only the severity of which varies.
Characteristic symptoms include pain, swelling, and functional difficulty. Clinical examination and imaging confirm the exact nature of your injury and determine its severity.
Can I walk with an ankle sprain?
This question comes up constantly. The answer depends on the severity of your sprain.
A mild sprain (grade 1) usually allows you to walk with moderate discomfort. You’re probably limping but you can support your weight. This functional capacity suggests that the ligaments, although stretched, maintain sufficient stability.
A moderate sprain (grade 2) makes walking difficult and painful. You could technically walk but at the cost of considerable effort and pronounced lameness. This early mobilization may aggravate partial ligament tears.
A severe sprain (grade 3) makes walking without support usually impossible. The intense pain and marked instability prevent normal loading. Forcing the walk in this situation prolongs healing and risks further damage to already compromised structures.
Dr. Émile Carrier, podiatrist and co-owner of our clinic, explains: “The ability to walk immediately after the injury does not guarantee the absence of a significant ligament fracture or tear. On the other hand, if you are unable to put weight on the affected ankle immediately after the accident, this is a great reason to see for x-rays to check for a fracture. If a fracture is identified, the treatment will be very different from that of a sprain. »
How long it takes to heal from an ankle sprain
The timeline of healing varies greatly depending on the severity of the sprain.
A mild sprain (grade 1) usually resolves in 1 to 3 weeks. The pain decreases quickly. The swelling gradually subsides. You are gradually returning to your normal activities.
A moderate sprain (grade 2) requires 3 to 6 weeks of recovery. The first few weeks often require protection with a splint or walking boot. Rehabilitation with amplitude and strengthening exercises becomes crucial to restore optimal function.
A severe sprain (grade 3) takes 8 to 12 weeks or more to heal completely. Strict initial immobilization protects torn ligaments while they heal. Gradual and supervised rehabilitation extends over several months to recover strength, proprioception and stability.
These delays represent the healing of the ligament tissues. Full functional recovery — including the return to demanding sports and activities — may require additional time.
Advanced Diagnosis at Our Clinic
Our on-site diagnostic capability speeds up your care and eliminates frustrating wait times.
Immediate digital radiography excludes associated fractures. Approximately 22% of ankle sprains are associated with fractures (references 1 and 2)—malleoli, base of the fifth metatarsal, posterior talus process. These fractures require separate management. You get this confirmation at your initial consultation.

Musculoskeletal ultrasound directly visualizes the injured ligaments. This technology evaluates the structural integrity of each ligament. It detects partial or complete tears. It identifies hematomas and periligament edema. This precise information guides our treatment recommendations.
The thorough clinical examination evaluates functional stability. Ligament stress tests. Joint range of motion assessment. Palpation of anatomical structures. This evaluation complements the imaging to establish the precise grade of your sprain.
How to heal an ankle sprain quickly?
Optimal healing is based on appropriate care from the first days.
The PEACE and LOVE protocol developed by physiotherapist Blaise Dubois and physiotherapist and researcher Jean-François Esculier has become our reference in the management of ankle sprains. The protocol is all about:
Acute phase: PEACE (the first few days)
P – Protection : Protect the injured area by limiting movements that increase pain during the first few days. Avoid activities that put excessive strain on injured ligaments, but without prolonged complete immobilization.
E – Elevation : Elevate your ankle above the level of the heart as often as possible. This position promotes the drainage of fluids and reduces swelling.
A – Avoid anti-inflammatories : Anti-inflammatory drugs and ice can interfere with the natural healing process in the long term. Inflammation is part of the tissue repair process. Prioritize pain management without blocking inflammation if it remains tolerable.
C – Compression : Use an elastic bandage to limit swelling and edema. Compression should be comfortable, never to the point of compromising circulation.
E – Education : Understand your wound and the healing process. Avoid excessive passive treatments and unnecessary imaging tests for mild sprains. Your body has a remarkable capacity for self-healing.
Recovery phase: LOVE (after the first few days)
L – Load : Gradually resume loading and movement as soon as the pain allows. The activity promotes tissue repair. Let the pain guide your progress — mild discomfort is okay, but the pain shouldn’t get worse.
O – Optimism : Maintain a positive attitude. Expectations and beliefs significantly influence recovery. Fear and catastrophization delay the return to normal activities.
V – Vascularization : Practice painless cardiovascular activities as soon as possible. Movement increases blood flow to injured tissue, speeding up healing. Walking, stationary cycling, swimming — choose activities that don’t cause significant pain.
E – Exercises : Quickly start mobility, strengthening and proprioception exercises. These exercises restore mobility, strength, and confidence in your ankle. Active rehabilitation far outperforms passive approaches.
Strict immobilization according to severity remains necessary for severe sprains during the initial phase. Mild sprains: support bandage or soft ankle braces. Moderate sprains: rigid splint or walking boot removable for a few weeks. Severe sprains: Stricter immobilization initially, followed by supervised progressive mobilization.
Dr. Sandra Gendron, podiatrist, emphasizes: “The PEACE and LOVE approach encourages the patient’s active participation in his or her healing. Proprioceptive exercises, in particular, are crucial for preventing recurrences. We guide this rehabilitation step by step, respecting your healing pace. »
Preventing Chronic Instability with Foot Orthotics
Approximately 40% of people with an ankle sprain develop chronic instability (Reference 3). This complication manifests itself in frequent recurrences, a persistent feeling of instability and limitation of activities.
Custom-made foot orthotics play a crucial role in preventing this chronic instability. These devices correct the underlying biomechanical imbalances that contributed to your initial sprain. A pronator foot (which sags inwards) places the ankle in a position vulnerable to lateral sprains. Orthotics stabilize your hindfoot, reducing this vulnerability.
We design your orthotics specifically for your unique biomechanics. Plantar arch support. Rearfoot stabilization. Correction of pressure imbalances. This personalized approach optimizes your protection in the long term.
Regular wear of orthotics, combined with strengthening and proprioception exercises, significantly reduces your risk of recurrence. This comprehensive strategy transforms an unstable ankle into a stable and functional joint.

When to consult for an ankle sprain?
Consult a doctor quickly if you cannot support your weight, if the swelling is significant, if the pain is severe or if you feel marked instability. Early professional evaluation differentiates between mild sprains and injuries requiring strict immobilization.
Access to on-site X-rays and ultrasound speeds up your diagnosis. You get answers and a treatment plan on your first visit. This effectiveness optimizes your healing and prevents long-term complications.
For a quick evaluation of your ankle sprain, make an appointment now by clicking hereor by calling 📞 819 800-1212
Podiatric consultations are NOT covered by the RAMQ. Private insurance usually covers our services. Documentation systematically provided for your complaints.